Prior Authorization Metrics
Centers for Medicare and Medicaid Services (CMS) Interoperability and Compliance Reporting
Fee for Service Medical Items and Services (excluding drugs)
Calendar Year 2025
To comply with the CMS Interoperability and Prior Authorization final rule, the Kentucky Department for Medicaid Services is required to annually report aggregated prior authorization metrics for fee-for-service on our website. This report includes data on the status of prior authorization requests, including approvals and denials, for the previous calendar year for fee-for-service from our waiver (Medicaid Waiver Management Application) and non-waiver (Essette) platforms.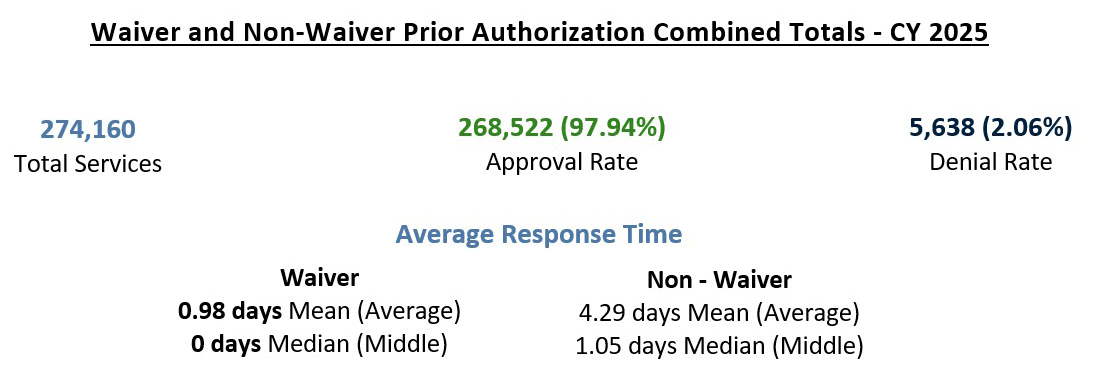
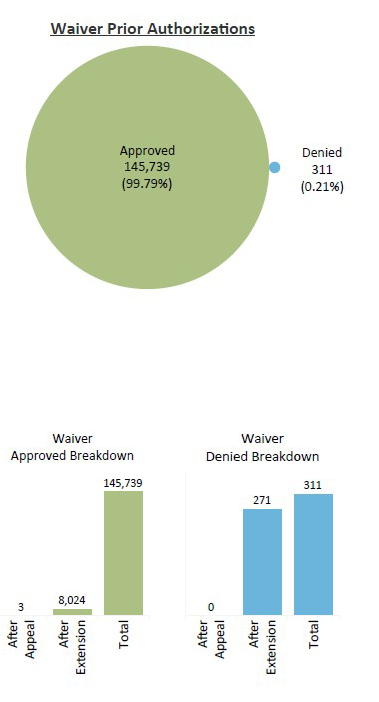
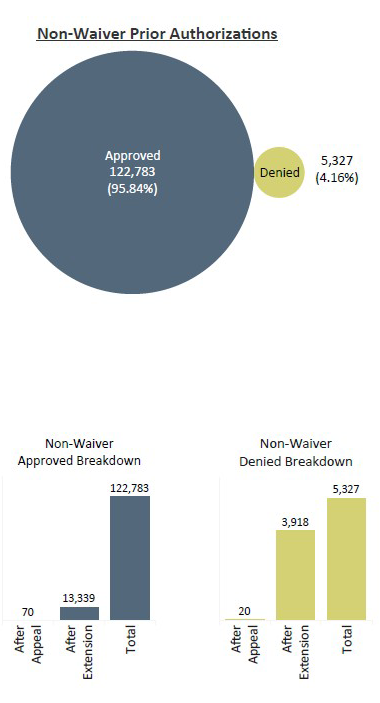
Lists of Services that Require Prior Authorization
Reporting Period: Calendar Year
Data Refresh Schedule: Yearly
Data Refresh Date: Feb. 24, 2026
Data Source: Utilization Management (UM) Prior Authorization (PA)
Medicaid Waiver Management Application (Vendor: Deloitte)
Essette (Vendor: Gainwell)
Note: A median time of 0.00 days indicates that the majority of requests received a decision within the same calendar day.